 OCTOBER 14, 2016
OCTOBER 14, 2016
Homoeopathy: What’s the harm in it? 02 Government criticism

GOVERNMENT OF AUSTRALIA: Homeopathy Review
Homeopathy is at best a placebo
https://www.nhmrc.gov.au/health-topics/complementary-medicines/homeopathy-review
05/03/2015
Homeopathy is a type of complementary and alternative medicine that is commonly used in Australia and around the world. NHMRC has reviewed the scientific evidence for the effectiveness of homeopathy in treating a variety of clinical conditions with the aim of providing Australians with reliable information about its use. The comprehensive assessment of the evidence included:
-a systematic review of the evidence from available systematic reviews (an overview) on the effectiveness of homeopathy in treating a variety of clinical conditions in humans
-a report on evidence submitted to the NHMRC prior to the commencement of the review
-a report on evidence submitted to the NHMRC during public consultation on the draft Information Paper; and
-consideration of published guidelines and other government reports.
The evidence identified in this assessment of the evidence has been summarised in a NHMRC Information Paper, which informed the development of NHMRC’s position on homeopathy. A NHMRC Statement has also been developed, based on the assessment of the evidence.
The NHMRC Information Paper and Statement, Administrative Report and the supporting evidence review reports, are available on the NHMRC website via the following links:
NHMRC Statement: Statement on Homeopathy
NHMRC Information Paper – Evidence on the effectiveness of homeopathy for treating health conditions
The Administrative Report provides a brief summary of the processes underpinning the homeopathy review, as well links to a number of additional documents:
Frequently Asked Questions arising from public consultation
Summary of key issues: Draft Information Paper on homeopathy—public consultation submissions
Summary of key issues: Draft Information Paper on homeopathy— expert review comments; and
A list of studies considered in the Overview and Review of submitted literature.
Homeopathy Working Committee
A Homeopathy Working Committee was established to guide the evidence review. The committee membership included researchers and experts in evidence-based medicine and complementary medicine.
More information about the Homeopathy Working Committee and its membership is available here.
Paul Glasziou: Still no evidence for homeopathy
http://blogs.bmj.com/bmj/2016/02/16/paul-glasziou-still-no-evidence-for-homeopathy/
February 16, 2016
When the National Health and Medical Research Council report on homeopathy concluded that “There was no reliable evidence from research in humans that homeopathy was effective for treating the range of health conditions considered” few in conventional medicine were surprised, but the homeopathy community were outraged. As chair of the working party which produced the report I was simply relieved that the arduous journey of sifting and synthesising the evidence was at an end. I had begun the journey with an “I don’t know” attitude, curious about whether this unlikely treatment could ever work. Still, who would have believed that bacteria caused peptic ulcers, or that vaccines for cancers would become routine.

So just maybe … but I lost interest after looking at the 57 systematic reviews (on 68 conditions) which contained 176 individual studies and finding no discernible convincing effects beyond placebo.
Of course, with 176 trials we would expect a few p-values under 5% just by chance: 1/20 of 176 is about 9 which luck would class as “statistically significant.” So we relied on replication and systematic reviews to avoid such false positives. The NHMRC did not redo all 63 systematic reviews (which at say $50,000 each would have cost over $3M), but appraised the existing reviews and used them as a window on the body of evidence. Though that body was mixed in size and quality, no clear signal of effectiveness emerged from the higher quality studies.
One surprise to me was the range of conditions that homeopathy had been evaluated in, including rheumatoid arthritis, radiodermatitis, stomatitis (inflammation of the mouth) due to chemotherapy, and human immunodeficiency virus (HIV) infection. What subsequently shocked me more was that organizations promote homeopathy for infectious conditions, such as AIDS in Africa or malaria. Given the current effective treatments, that seems a very dubious activity, and is another example that justifies the NHMRC statement that “People who choose homeopathy may put their health at risk if they reject or delay treatments for which there is good evidence for safety and effectiveness.”
Unsurprisingly there has been considerable pushback from those who use or sell homeopathic remedies. Indeed the International Council for Homeopathy is currently leading a fund-raising effort: not to fund better research, but to attack the NHMRC document. I can well understand why Samuel Hahnemann—the founder of homeopathy—was dissatisfied with the state of 18th century medicine’s practices, such as blood-letting and purging, and tried to find a better alternative. But I would guess he would be disappointed by the collective failure of homeopathy to carry on his innovative investigations, but instead continue to pursue a therapeutic dead-end.
Paul Glasziou is professor of evidence based medicine at Bond University and a part time general practitioner. He chaired the NHMRC report on homeopathy
Readers’ comments
1. Prof Glasziou, I’ve been washing a homeopathy bottle every day for the last month, but the residue just keeps on getting stronger. Any advice? –Simon Chapman
2. How do homeopaths test the “remedies” they buy from wholesalers? How can they be sure they are not being sold just plain water? –Matt Walker-Wilson
3. They don’t. They can’t tell the difference. Only the label is different. But no need to take my word for it:
House of Lords Science and Technology Committee 21 FEBRUARY 2007
Ms. Chatfield: I am Kate Chatfield. I am here to represent the Society of Homeopaths and I am a senior lecturer in homeopathy at the University of Central Lancashire.
Q538 Lord Broers: I have a simple, technical question about homeopathy and drugs. Is it possible to distinguish between homeopathic drugs after they have been diluted? Is there any means of distinguishing one from the other?
Ms. Chatfield: Only by the label.
http://www.publications.parliament.uk/…
–Allan Henness
GOVERNMENT OF U.K.: Homeopathy
http://www.nhs.uk/conditions/Homeopathy/Pages/Introduction.aspx
National Health Services, U.K., February 15, 2015
Introduction
Homeopathy is a ‘treatment’ based on the use of highly diluted substances, which practitioners claim can cause the body to heal itself.
A 2010 House of Commons Science and Technology Committee report on homeopathy said that homeopathic remedies perform no better than placebos, and that the principles on which homeopathy is based are “scientifically implausible”*. This is also the view of the Chief Medical Officer, Professor Dame Sally Davies.
This page covers:
What should I expect if I try it?
What are the regulation issues?
What can we conclude from the evidence?
What is homeopathy?
Homeopathy is a complementary or alternative medicine (CAM)*. This means that homeopathy is different in important ways from treatments that are part of conventional Western medicine*.
It is based on a series of ideas developed in the 1790s by a German doctor called Samuel Hahnemann.
A central principle of the “treatment” is that “like cures like” – that a substance that causes certain symptoms can also help to remove those symptoms. A second central principle is based around a process of dilution and shaking, called succussion.
Practitioners believe that the more a substance is diluted in this way, the greater its power to treat symptoms. Many homeopathic remedies consist of substances that have been diluted many times in water until there is none or almost none of the original substance left. Homeopathy is used to “treat” an extremely wide range of conditions, including physical conditions such as asthma and psychological conditions such as depression (see When is it used?).
Does it work?
There has been extensive investigation of the effectiveness of homeopathy. There is no good-quality evidence that homeopathy is effective as a treatment for any health condition (see What can we conclude from the evidence?).
It is available on the NHS?
Homeopathy is not available on the NHS in all areas of the country. Two NHS hospitals provide homeopathy, and some GP practices also offer it.
Homeopathy is usually practised privately and homeopathic remedies are available from pharmacies. The price for an initial consultation with a homeopath can vary from around £20 to £80. Homeopathic tablets or other products usually cost around £4 to £10.
What should I expect if I try it?
When you first see a homeopath they will usually ask you about any specific health conditions, but also about your general wellbeing, emotional state, lifestyle and diet.
Based on this, the homeopath will decide on the course of treatment, which most often takes the form of homeopathic remedies given as a pill, capsule or tincture.
Your homeopath may recommend that you attend one or more follow-up appointments so the effects of the remedy on your health can be assessed.
When is it used?
Homeopathy is used for an extremely wide range of health conditions. Many practitioners believe that homeopathy can help with any condition.
Among the most common conditions that people seek homeopathic treatment for are:
asthma
ear infections
hay fever
mental health conditions, such as depression, stress and anxiety
allergies, such as food allergies
dermatitis (an allergic skin condition)
arthritis
high blood pressure
There is no good quality evidence that homeopathy is an effective treatment for these or any other health conditions. Some practitioners also claim that homeopathy can prevent malaria or other diseases. There is no evidence to support this and no scientifically plausible way that homeopathy can prevent diseases.
The National Institute of Health and Care Excellence (NICE) advises the NHS on proper use of treatments. NICE currently does not recommend that homeopathy should be used in the treatment of any health condition.
What are the regulation issues?
There is no legal regulation of homeopathic practitioners in the UK. This means that anyone can practise as a homeopath, even if they have no qualifications or experience. Voluntary regulation aims to protect patient safety, but it does not mean that there is scientific evidence that a treatment is effective.
A number of professional associations can help you to find a homeopath who will practise the treatment in a way that is acceptable to you.
The Society of Homeopaths and the Federation of Holistic** Therapists both have a register of homeopathy practitioners, which you can search to find a practitioner near you. These registers are accredited by the Professional Standards Authority.
*In other words, it is New Age. That is the reason why it is in the list of alternative therapies in the February 3, 2003, Vatican Document on the New Age #2.2.3, though Catholic practitioners prefer to ignore the truth.
**The Document also speaks about the New Age paradigm of holistic health, #2.2.3, #2.2.4, 2.4, 4 etc.
Is it safe?
Homeopathic remedies are generally safe and the risk of a serious adverse side effect arising from taking these remedies is thought to be small.
Some homeopathic remedies may contain substances that are not safe, or that interfere with the action of other medicines. You should talk to your GP before stopping any treatment prescribed by a doctor or avoiding procedures such as vaccination in favour of homeopathy.
What can we conclude from the evidence?
There have been several reviews of the scientific evidence on the effectiveness of homeopathy. The House of Commons Science and Technology Committee said there is no evidence that homeopathy is effective as a treatment for any health condition.
There is no evidence for the idea that substances that can induce certain symptoms can also help to treat them. There is no evidence for the idea that diluting and shaking substances in water can turn those substances into medicines.
The ideas that underpin homeopathy are not accepted by mainstream science, and are not consistent with long-accepted principles on the way that the physical world works. The Committee’s 2010 report on homeopathy said the “like cures like” principle is “theoretically weak”, and that this is the “settled view of medical science”.
It is of note, for example, that many homeopathic remedies are diluted to such an extent that there is unlikely to be a single molecule of the original substance remaining in the final remedy. In cases such as these, homeopathic remedies consist of nothing but water.
Some homeopaths believe that, due to the succussion process, the original substance leaves an “imprint” of itself on the water. But there is no known mechanism by which this can occur. The 2010 report said: “We consider the notion that ultra-dilutions can maintain an imprint of substances previously dissolved in them to be scientifically implausible.”
Some people who use homeopathy may see an improvement in their health condition due to a phenomenon known as the placebo effect.
If you choose health treatments that provide only a placebo effect, you may miss out on other treatments that have been proven to be more effective.
GOVERNMENT OF U.K.: The placebo effect and complementary and alternative medicine (CAM)
http://www.nhs.uk/livewell/complementary-alternative-medicine/pages/placebo-effect.aspx
National Health Services, U.K., February 3, 2016
When a person uses any type of health treatment and sees an improvement in their symptoms, they may be experiencing the placebo effect.
For hundreds of years, doctors have known that when a patient with a health condition expects their symptoms to improve, they often do improve.
Today, we know that patients who are given empty injections or pills that they believe contain medicine can experience an improvement in a wide range of health conditions.
This kind of fake or empty medicine is often called a “placebo”, and the improvement this causes is called the “placebo effect”.
It can affect all of us and can occur when a person uses any kind of health treatment – either conventional or complementary and alternative.
It’s important to be aware of the placebo effect when choosing complementary and alternative medicines (CAMs).
If you choose a complementary or alternative treatment that does not work – and only causes a placebo effect – you may miss out on more effective treatments.
This page covers:
Examples of the placebo effect
Checking the evidence for or against a treatment
Examples of the placebo effect
One well-known example of the placebo effect involves a physical feeling we are all familiar with: pain.
In 1996, scientists assembled a group of students and told them that they were going to take part in a study of a new painkiller, called “trivaricaine”. Trivaricaine was a brown lotion to be painted on the skin, and that smelled like a medicine. But the students were not told that, in fact, trivaricaine contained only water, iodine and thyme oil – none of which are painkilling medicines. It was a fake – or placebo – painkiller.
With each student, the trivaricaine was painted on one index finger, and the other left untreated. In turn, each index finger was squeezed in a vice. The students reported significantly less pain in the treated finger, even though trivaricaine was a fake.
In this example, expectation and belief produced real results. The students expected the “medicine” to kill pain; and, sure enough, they experienced less pain. This is the placebo effect.
Read a summary of the study: Mechanisms of Placebo Pain Reduction.
Placebo medicine has even been shown to cause stomach ulcers to heal faster than they otherwise would.
These amazing results show that the placebo effect is real, and powerful. They mean that fake or placebo treatments can cause real improvements in health conditions. Experiencing the placebo effect is not the same as being “tricked”, or being foolish. The effect can happen to everyone, however intelligent, and whether they know about the placebo effect or not.
CAM and the placebo effect
Evidence about a treatment is gathered by conducting fair tests. In these tests, scientists find out whether a treatment causes an improvement beyond the improvement caused by the placebo effect alone.
Evidence plays an important role in mainstream medicine. This means that when you use many conventional medicines, you can be sure there is evidence they work.
When patients experience improvement after using a healthcare treatment that has not been proven to work, they may only be experiencing the placebo effect. Of course, improvement in a health condition due to the placebo effect is still improvement, and that is always welcome. But it is important to remember that for many health conditions, there are treatments that work better than placebos. If you choose a treatment that only provides a placebo effect, you will miss out on the benefit that a better treatment would provide.
Checking the evidence for or against a treatment
The only way to know whether a health treatment works better than a placebo treatment is by checking the evidence.
Evidence, CAM and the NHS
The National Institute for Health and Care Excellence (NICE) uses evidence when it draws up guidance for the NHS on the use of treatments and the care of patients. Currently, NICE recommends the use of a complementary and alternative treatment in a limited number of instances, including:
Alexander Technique* for Parkinson’s disease
Ginger and acupressure* for reducing morning sickness
Acupuncture* and manual therapy for low back pain
You can read about the evidence for different CAMs on pages about specific treatments. See our index for a list of all treatments covered by NHS Choices.
How evidence is gathered and used
The best way to produce good evidence on a health treatment is to conduct a fair test. Here, the medicine or treatment being tested is compared to another treatment, or to a placebo.
Tests are made as fair as possible by minimising bias and the role of chance. This means that the test results will reflect, as far as possible, the truth about the medicine or treatment, and will not be influenced by other factors, such as the way the test was carried out, or the attitudes of the people who take part.
Scientists often call these fair tests clinical trials.
Before scientists conclude that a health treatment is safe and that it works, there must usually have been several independent tests of the treatment that have shown this.
Sometimes, different fair tests can give results that disagree.
The results of fair tests can provide:
results that show the medicine or treatment does work and is safe; this is often call positive evidence, or evidence for the treatment
results that show the medicine does not work, or is unsafe; this is often called negative evidence, or evidence against the treatment
Negative evidence – that is, evidence against a treatment – is not the same as no evidence. Negative evidence means a set of results showing that a medicine or treatment does not work.
No evidence simply means an absence of any evidence, because fair tests have not been conducted.
Where to find out more
Read about the evidence for different CAMs on pages about specific treatments. See our index for a list of all treatments covered by NHS Choices.
Search for evidence on any treatment on the NHS Evidence
website.
More articles on: Complementary and alternative medicine
CAMs like homoeopathy: Physically safe, but useless, a placebo. A practitioner might be cheating a patient out of proper and timely effective conventional medical care.
For Christians, spiritually unsafe, New Age philosophies. Best to avoid.
*Alexander Technique is New Age: http://ephesians-511.net/docs/ALEXANDER_TECHNIQUE.doc.
Acupuncture is in the list of therapies in “Jesus Christ the Bearer of the Water of Life”.
Watch
https://www.youtube.com/watch?v=HMGIbOGu8q0
2:33 and have a good laugh.
Wikipedia founder calls alt-medicine practitioners “lunatic charlatans”
Wales to activists who want new rules for Wikipedia: “No, you have to be kidding me.”
By Megan Geuss, March 26, 2016
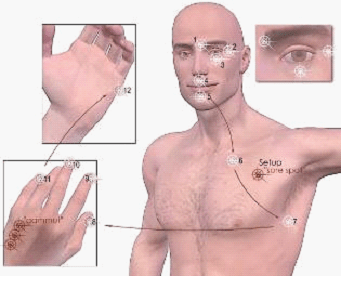
A diagram about Emotional Freedom Techniques that is hosted on Wikipedia
[EMOTIONAL FREEDOM TECHNIQUE
http://ephesians-511.net/docs/EMOTIONAL_FREEDOM_TECHNIQUE.doc]
Several months ago, the Association for Comprehensive Energy Psychology (ACEP), an alternative medicine non-profit, began a petition on Change.org asking Wikipedia to “create and enforce new policies that allow for true scientific discourse about holistic approaches to healing.” The petition reached 7,000 signatures in mid-January and then largely stalled. But this weekend, Wikipedia co-founder Jimmy Wales responded to the request, saying that no amount of signatures would get him on board with ACEP’s request.
In its petition, ACEP wrote to Wikipedia, “people who are interested in the benefits of Energy Medicine***, Energy Psychology, and specific approaches such as the Emotional Freedom Techniques, Thought Field Therapy, and the Tapas Acupressure Technique, turn to your pages, trust what they read, and do not pursue getting help from these approaches which research has, in fact, proven to be of great benefit to many.”
“These pages are controlled by a few self-appointed ‘skeptics’ who serve as de facto censors for Wikipedia,” the petition continued. “They clothe their objections in the language of the narrowest possible understanding of science in order to inhibit open discussion of innovation in health care.” As of this writing, another 800 people have signed the petition in support of a revision of Wikipedia’s policies.
Our house, our rules
Wales, however, responded on Change.org with a short note:
“No, you have to be kidding me. Every single person who signed this petition needs to go back to check their premises and think harder about what it means to be honest, factual, truthful.
Wikipedia’s policies around this kind of thing are exactly spot-on and correct. If you can get your work published in respectable scientific journals—that is to say, if you can produce evidence through replicable scientific experiments, then Wikipedia will cover it appropriately.
What we won’t do is pretend that the work of lunatic charlatans is the equivalent of “true scientific discourse.” It isn’t.”
Wikipedia’s guidelines for the inclusion of information are outlined at length on its project pages, but the ACEP did not identify a specific rule it wanted added or excised in its grievances. (The ACEP has not yet responded to Ars Technica’s* request for comment. This article will be updated if we hear back.)
One rule that may have irked alternative medicine proponents might be that Wikipedia tries to avoid being the host of original perspectives. As the site states on one project page, “Wikipedia does not publish original thought: all material in Wikipedia must be attributable to a reliable, published source.”
The website also may not accept some of the sources that the alternative practitioners rely on. It insists that editors “Base articles on reliable, third-party, published sources with a reputation for fact-checking and accuracy… The best sources have a professional structure in place for checking or analyzing facts, legal issues, evidence, and arguments. The greater the degree of scrutiny given to these issues, the more reliable the source. Be especially careful when sourcing content related to living people or medicine.”
In its content guidelines, Wikipedia has a whole page dedicated to fringe theories and makes it clear that subjects like alternative medicine will be treated as such. “A theory that is not broadly supported by scholarship in its field must not be given undue weight in an article about a mainstream idea, and reliable sources must be cited that affirm the relationship of the marginal idea to the mainstream idea in a serious and substantial manner.”
Bunk science maybe, but let’s talk about it
Interestingly, the petition also cited Wikipedia co-founder Larry Sanger, who has since left the project, as proof that the site needed an overhaul of its policies:
“Larry Sanger, co-founder of Wikipedia, left the organization due to concerns about its integrity. He stated: “In some fields and some topics, there are groups who ‘squat’ on articles and insist on making them reflect their own specific biases. There is no credible mechanism to approve versions of articles.”
This is exactly the case with the Wikipedia pages for Energy Psychology, Energy Medicine, acupuncture, and other forms of complementary/alternative medicine (CAM), which are currently skewed to a negative, unscientific view of these approaches despite numerous rigorous studies in recent years demonstrating their effectiveness.”
Ars Technica contacted Sanger about the use of his name in this argument, and he offered a more nuanced take on the petitioners’ request:
“Wikipedia’s neutrality policy, at least as I originally articulated it, requires that CAM’s practitioners be given an opportunity to explain their views. At the same time, the policy also requires that more space be given to mainstream views that are critical of CAM, precisely because such critical views are held by most medical health professionals.
…
I am as big a defender of rationality, science, and objective reality as you are likely to find. But I also think a public resource like Wikipedia should be fully committed to intellectual tolerance and the free exchange of ideas. That, together with an interest in providing a way to resolve disputes, is just what drove me to advocate for and articulate the Wikipedia’s neutrality policy. I have confidence that if CAM’s advocates are given an opportunity to air their views fully and sympathetically—not to say they should be allowed to make Wikipedia assert their views—and skeptics are also given free rein to report their explanation of why they think CAM is a load of crap, then a rational reader will be given the tools he or she needs to take a reasonable position about the matter.”
Putting all ideas on the table—but giving more space to the mainstream views and putting less emphasis on the alternative views—might be problematic in practice. Requiring that Wikipedia sources be based on third-party, published, and often peer-reviewed work is an easy way to at least make a passing effort at disseminating high-quality information. But how would space be doled out to advocates of alternative theories, who are just as certain about the rightness of their ideas as any scientist, if that guideline became more flexible? Would they be allowed to present their views in a set number of paragraphs? Or as a percentage of the number of words written about mainstream theories? Such a setup might be a slippery slope to what’s been termed “false balance,” a subject on which Ars has written at length before. In that scenario, views that have been ignored for a reason are given undeserved light to create the illusion of an even playing field.
If you’d like Ars’ take on alternative medicine, check out our long explainer on homeopathy and pseudoscience.
***Homoeopathy classifies as “energy medicine” as it allegedly works on the “vital” or “subtle” energy body of the patient
5 HOMOEOPATHY REPORTS
HOMOEOPATHY CONTROVERSY AND FR RUFUS PEREIRA
http://ephesians-511.net/docs/HOMOEOPATHY_CONTROVERSY_AND_FR_RUFUS_PEREIRA.doc
HOMOEOPATHY INSTITUTIONALIZED IN THE INDIAN CATHOLIC CHURCH
http://ephesians-511.net/docs/HOMOEOPATHY_INSTITUTIONALIZED_IN_THE_INDIAN_CATHOLIC_CHURCH.doc
INSTITUTIONALIZED NEW AGE IN BOMBAY ARCHDIOCESE-HOMOEOPATHY, YOGA AND KRIPA FOUNDATION
HOMOEOPATHY-BBC-THE TEST
http://ephesians-511.net/docs/HOMOEOPATHY-BBC-THE_TEST.doc
HOMOEOPATHY IS BUNK-INDIAN NOBEL LAUREATE
http://ephesians-511.net/docs/HOMOEOPATHY_IS_BUNK-INDIAN_NOBEL_LAUREATE.doc
12 HOMOEOPATHY ARTICLES/COLLATIONS
AYUSH-THE NEW AGE DANGERS OF
http://ephesians-511.net/docs/AYUSH_THE_NEW_AGE_DANGERS_OF.doc
HOMOEOPATHY-AN UNSCIENTIFIC NEW AGE FRAUD
http://ephesians-511.net/docs/HOMOEOPATHY-AN_UNSCIENTIFIC_NEW_AGE_FRAUD.doc
HOMOEOPATHY-AN UNSCIENTIFIC NEW AGE FRAUD 02
http://ephesians-511.net/docs/HOMOEOPATHY-AN_UNSCIENTIFIC_NEW_AGE_FRAUD_02.doc
HOMOEOPATHY-AN UNSCIENTIFIC NEW AGE FRAUD 03
http://ephesians-511.net/docs/HOMOEOPATHY-AN_UNSCIENTIFIC_NEW_AGE_FRAUD_03.doc
*HOMOEOPATHY-ARS TECHNICA
http://ephesians-511.net/docs/HOMOEOPATHY-ARS_TECHNICA.doc
HOMOEOPATHY-DR EDWIN A NOYES
http://ephesians-511.net/docs/HOMOEOPATHY-DR_EDWIN_A_NOYES.doc
HOMOEOPATHY-ERIKA GIBELLO
http://ephesians-511.net/docs/HOMOEOPATHY-ERIKA_GIBELLO.doc
HOMOEOPATHY-FR CLEMENS PILAR 10
http://ephesians-511.net/docs/HOMOEOPATHY-FR_CLEMENS_PILAR_10.doc
HOMOEOPATHY-SUMMARY
http://ephesians-511.net/docs/HOMOEOPATHY-SUMMARY.doc
HOMOEOPATHY-SUSAN BRINKMANN
http://ephesians-511.net/docs/HOMOEOPATHY-SUSAN_BRINKMANN.doc
HOMOEOPATHY-WHAT’S THE HARM IN IT?
http://ephesians-511.net/docs/HOMOEOPATHY-WHATS_THE_HARM_IN_IT.doc
HOMOEOPATHY LAMPOONED
http://ephesians-511.net/docs/HOMOEOPATHY_LAMPOONED.doc
1 HOMOEOPATHY TESTIMONY
TESTIMONY OF A FORMER HOMOEOPATHY PRACTITIONER-01 DR. EMILIA VLCKOVA
http://ephesians-511.net/docs/TESTIMONY_OF_A_FORMER_HOMOEOPATHY_PRACTITIONER-01.doc
Categories: Alternative Therapy, new age
 FRANCIS WON’T ABOLISH ‘HINDU RITE’ EUCHARIST
FRANCIS WON’T ABOLISH ‘HINDU RITE’ EUCHARIST  “Compendium of New Age Deceptions and Corresponding Church Teachings: Medications and Meditations in the New Age” Book Author – Michael Prabhu
“Compendium of New Age Deceptions and Corresponding Church Teachings: Medications and Meditations in the New Age” Book Author – Michael Prabhu  Bangalore priest Fr. Adrian Mascarenhas flays my Open Letter on the Amazon Synod to Cardinal Oswald Gracias 02
Bangalore priest Fr. Adrian Mascarenhas flays my Open Letter on the Amazon Synod to Cardinal Oswald Gracias 02  Bangalore priest Fr. Adrian Mascarenhas flays my Open Letter on the Amazon Synod to Cardinal Oswald Gracias
Bangalore priest Fr. Adrian Mascarenhas flays my Open Letter on the Amazon Synod to Cardinal Oswald Gracias
Leave a comment